Veterinary antibiogram testing: what it is and when to use it

Veterinary antibiogram testing: what it is and when to use it
Antibiotic decisions in small-animal practice are rarely made in ideal conditions. A dog with recurrent otitis, a cat with suspected bacterial cystitis, or a patient with a non-healing skin infection often needs a treatment plan despite an incomplete picture.
In these situations, microbiological testing can be highly useful. Clinical presentation, cytology, urinalysis, and patient history all help guide the decision, but they do not always reliably show whether a bacterial pathogen is present or which antimicrobial is likely to work.
This is where veterinary antibiogram testing adds value. It helps confirm bacterial involvement, identifies which antimicrobials are likely to inhibit the organism in vitro, and provides the clinician with a stronger basis for moving from empirical treatment toward a more targeted choice.
It is not a replacement for clinical judgment. Site of infection, drug penetration, patient factors, previous treatment, topical versus systemic therapy, dosing, safety, owner constraints, and local guidelines still matter. But when bacterial infection is plausible, and the antibiotic choice is uncertain, an antibiogram can make the decision more defensible.
What is an antibiogram in veterinary practice?
In everyday clinical language, "antibiogram" refers to the antimicrobial susceptibility results for a specific patient sample. The lab grows the bacterial isolate, tests it against selected antimicrobials, and reports whether each option is interpreted as susceptible, susceptible with increased exposure ("intermediate"), or resistant according to the relevant method and breakpoint framework (EUCAST and CLSI).
The broader technical term is antimicrobial susceptibility testing, or AST. AST can be performed using methods such as disk diffusion or broth microdilution. The important point for the clinician is that the method must be standardized, quality-controlled, and interpreted with appropriate veterinary criteria where available.
The 2023 review of veterinary AST by Fessler and colleagues in One Health Advances emphasizes that veterinary AST is complex and must adhere to published methods, expert oversight, and appropriate interpretive criteria. If methods, incubation conditions, breakpoints, or quality controls are wrong, there is a practical risk for clinics that antibiograms might not be reliable.
When should a clinic consider performing an antibiogram?
Antibiogram testing is most useful when the result can change the clinician's next steps.
Strong use cases include recurrent infections, non-responsive infections, recent antimicrobial exposure, plausible resistant organisms, cases where broad-spectrum or high-importance antimicrobials are being considered, and cases where the clinic wants to document stewardship-aligned decision-making.
The 2022 AAFP/AAHA Antimicrobial Stewardship Guidelines position diagnostics as part of sensible prescribing, not as an academic extra. Their practical message is that stewardship in companion animals depends on accurate diagnosis, responsible antimicrobial use, monitoring response, and client education.
In other words, the decision is not simply "test everything" or "treat everything empirically." The right question is: Will this test reduce uncertainty enough to improve the treatment plan?
Urinary tract infections
UTIs, urinary tract infections (especially cystitis), are a high-value area for culture and susceptibility testing. A cytological urine analysis is not reliable in confirming bacterial presence; thus, standard culture and susceptibility testing shall guide antimicrobial selection when treatment is indicated.
The ISCAID urinary tract infection guidance for dogs and cats recommends culture and susceptibility testing in important scenarios, including upper urinary tract infection and more complicated situations. Recent studies of canine and feline urinary isolates continue to show that resistance patterns vary and that susceptibility data can matter, particularly in recurrent or previously treated cases.
Skin infections
Skin infections are a common reason for antibiotic use in dogs and cats, but not every inflamed skin lesion needs systemic antimicrobial therapy. Cytology, lesion type, severity, recurrence, and underlying disease all matter.
Antibiogram testing becomes more valuable when infection is recurrent, deep, non-responsive, or when previous antimicrobial exposure raises concern for resistance. In those cases, culture and AST can help the clinician avoid repeated trial-and-error prescribing and can support a more targeted plan.
Ear infections
Otitis externa is one of the most practical examples of why AST needs clinical context. Many ear infections involve mixed factors: anatomy, allergy, moisture, biofilm, yeast, bacteria, chronic inflammation, and owner compliance. Cytology and otoscopic findings still sit at the center of the workup.
Culture and susceptibility testing can be especially useful in chronic, recurrent, severe, or non-responsive bacterial otitis, particularly when Pseudomonas or multidrug-resistant staphylococci are suspected.
The nuance is that AST is primarily designed to predict systemic antimicrobial activity. Topical ear therapy can reach concentrations that are not directly reflected by a standard systemic breakpoint. That does not make culture and AST useless in otitis. It means the veterinarian should interpret the result in light of cytology, topical options, ear canal status, patient history, and clinical response.
Why reporting style matters
How an AST result is displayed affects prescribing behavior. A long list of susceptible antibiotics can push clinicians toward options that are broader than needed. Cascade reporting addresses this by showing first-line choices first and revealing broader options only when needed.
VetBac's existing article on AST reporting discusses evidence that cascade-style reports can improve guideline-aligned decision-making in small-animal medicine.
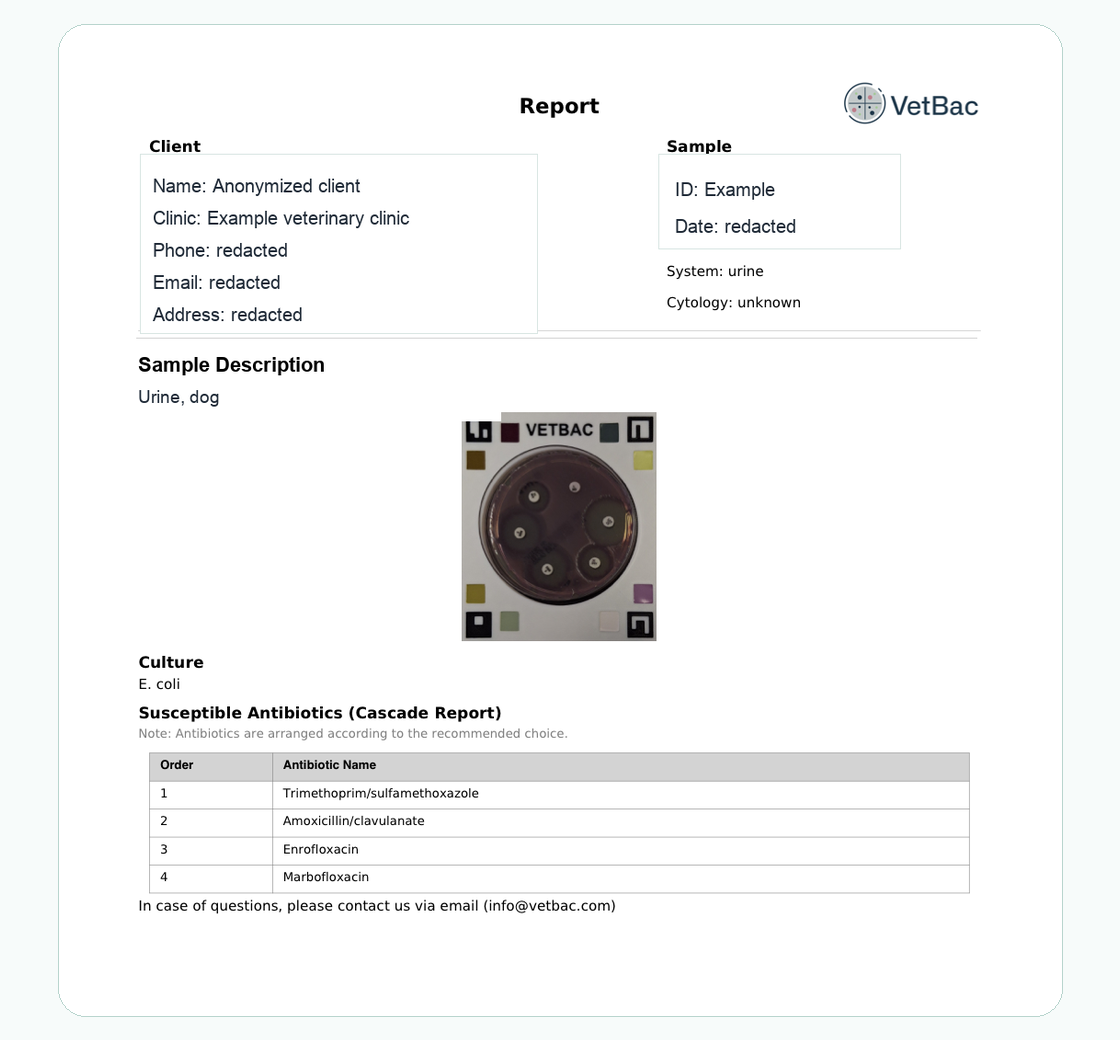 Figure 1. VetBac report example showing culture, plate image, and prioritized antibiotic options.
Figure 1. VetBac report example showing culture, plate image, and prioritized antibiotic options.
How in-clinic next-day testing changes the workflow
Traditional send-out culture and susceptibility workflows can be clinically valuable, but timing can be hard. The sample has to leave the clinic, the lab has to process it, the result has to return, and the clinician has to reconnect that result to the case.
An in-clinic next-day workflow changes the decision timeline. Instead of treating empirically for several days before receiving microbiology data, the clinic can run testing close to the patient encounter and use the results earlier in the case.
Practical checklist
Before ordering or running veterinary antibiogram testing, ask:
- Is bacterial infection clinically plausible?
- Has cytology, urinalysis, or another first-line diagnostic test supported the suspicion?
- Would the result change the antimicrobial choice, route, or decision to treat?
- Is this recurrent, severe, non-responsive, or previously treated?
- Are broad-spectrum or high-importance antimicrobials being considered?
- Will the report be interpreted with clinical context rather than as an automatic prescription list?
If the answer to several of these is yes, AST is more likely to add value.
Bottom line
Veterinary antimicrobial susceptibility testing is most useful when it helps the clinician move from uncertainty to a better-supported treatment decision. It is not just a lab output. It is part of a stewardship workflow: diagnose carefully, test when the result matters, interpret in context, and choose antimicrobials deliberately.
VetBac is built around that workflow: next-day in-clinic antibiogram testing, clear reporting, and microbiology support for small-animal practices treating common bacterial infections. For canine-specific guidance, see our article on culture and sensitivity testing in dogs. To learn how we validate our testing media, see how we perform quality control.
Sources
- Fessler et al., Antimicrobial susceptibility testing in veterinary medicine: performance, interpretation of results, best practices and pitfalls, One Health Advances, 2023.
- 2022 AAFP/AAHA Antimicrobial Stewardship Guidelines.
- EUCAST VetCAST.
- ISCAID guidelines for bacterial urinary tract infections in dogs and cats.
Explore More Veterinary Insights
Ready to improve your antibiogram testing?
Get overnight results with clear, actionable reports.
Book a demo